Site visit: Birmingham goes paperless in ICU
- 3 November 2016

Serving the nation’s second city, University Hospitals Birmingham NHS Foundation Trust has to be prepared to provide direct clinical care for 800,000 patients, while being a world renowned centre for organ transplant, trauma and kidney care.
To support its expertise in clinical care, the trust has been red hot on data management and electronic systems.
It has been developing its own award winning, in-house prescribing information and communication system or PICS since1999, and was recently announced as one of the first round of global digital centres of excellence, or exemplars.
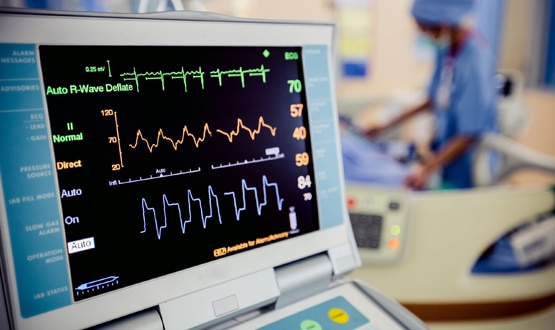
At the Queen Elizabeth Hospital Birmingham, there is a huge intensive care unit with 100 bed spaces, spread across four wards. Since May this year, it has been implementing an electronic version of the traditional paper chart found at the end of a patient’s bed.
Replacing the paper chart
Entering the ICU, the corridor stretches away into the distance. There are nurses scribbling over huge, highly detailed A0 bits of paper and then, in another ward, typing away at equally large, washable keyboards.
The electronic paper chart is undergoing its phased roll out, following a successful pilot earlier in the year. It is currently in three units, with the fourth due over the next few months.
Logging in, Helen Gyves, lead nurse for clinical IT, shows how all the patient’s information is accessible not only in the ward, but also remotely. It makes the history of the patient much more accessible, because it’s no longer necessary to go digging through piles of paper to find it.
The system can pre-empt the end of an order, which means less data entry for the user. The exact numbers show that recording complex data takes an average of 1 minute 40 seconds on the electronic device, in comparison to 2 minutes 5 seconds on paper.
The system can also do drug calculations, and provide decision support. Gyves shows how advising symbols (for example end of life, do not resuscitate, pharmacist approved drugs) can have messages attached to them, which flash up when hovered over.
And by replacing the paper chart, there are no longer queries about dubious handwriting, something appreciated by the local coroner. In 2014, a Care Quality Commission report found at Manchester Royal Infirmary that doctors’ illegible scrawling could be putting patients at risk.
What does the front line say?
Often, it seems that trusts implement technology from the top down, and when it reaches the coal face it is not wanted nor used. This lack of communication was highlighted in Robert Wachter’s report on NHS IT, which said clinical involvement in the development and deployment of systems is vital to success.
Birmingham has tried to get out ahead of this issue by appointing a nurse in a leading role for deploying the technology in the ICU. This clinician focused approach is supported by Clare Strivens, a senior sister on the ICU ward.
“It’s a lot quicker and a lot easier,” Strivens says about the new system; laughing when Gyvens looks surprised. While it took a while to get used to, she adds, as a nurse in charge it’s very useful for seeing what is going on; calculations are quicker and there can be instant follow up.
Keeping it all in-house with PICS
While the ICU has gone from paper based charts to electronic working, the PICS has been around for a long time. When it first came in, Gyves remembers: “We did have some nurses leave who were so frightened of having an IT tool to do the job they had done on a piece of paper for so many years”.
However, that’s now a fading memory. PICS has successfully increased compliance with prescribing from 50% to 95% over two and half years and created a 17% reduction in the mortality rate in Birmingham in comparison to standardised mortality ratios throughout England.
In fact, Gyves adds, the downside is that everyone wants everything in PICS now, so the challenge has become trying to manage people’s expectations.
This includes the other trusts in Birmingham. Birmingham Children’s Hospital NHS Foundation Trust is in the process of implementing its own e-prescribing system by next year, having added specialist paediatric drugs to the library.
The Royal Orthopaedic Hospital NHS Foundation Trust is also in discussions to implement PICS and the neighbouring troubled Heartlands Hospital is receiving the IT system.
Big Brother is watching you
One of the factors behind the e-prescribing and HSMR improvements is the data rich environment that clinicians work in. By monitoring health professionals using the system, bad habits can be nipped in the bud early.
Suzy Gallier, clinical business development lead at Birmingham, says there was some initial reluctance around this, as it was a bit “big brother is watching you”. But because the data is there in black and white, practice can be challenged with evidence; there’s no chance of a ‘you did this, no I didn’t’ situation developing.
As a huge teaching hospital, Queen Elizabeth’s junior doctors have benefited from this. In a comment piece on National Health Executive, the trust’s executive director of delivery, Tim Jones estimated that 20,000 errors are prevents by junior doctors annually thanks to Birmingham’s IT systems.
Checks and balances
Data can also be used proactively. Information from PICS is used for everything from identifying infectious patients to medical research.
But with so much personal data – including details of friends, families and colleagues – within the trust’s extensive database information governance and security has to be an issue.
“It’s like giving someone a blank cheque,” says Gyves; and consequently there is an extremely tight policy on the misuse of IT, with job loss as a possible consequence.
Blackberries in the ICU
The ICU technology is fully integrated with PICS, and while the paperless charts are at data entry level currently, the next phase will be to add in alerts.
Another plan for the ICU is to give the nurses in charge a BlackBerry device. When a doctor prescribes an antibiotic, an alert will be sent through to say that has been done, to make sure it is administered. It will also register a pain score, so if a patient is in agony with no pain killer then the lead nurse can be notified.
For Gyves, these developments are something that she is delighted to be a part of. “As a nurse, my priority should be my patient, so if you can show me my patient is getting a better deal, and I believe it, I’m going to go with that.”