A few of you might recall that a couple of years ago I suggested that pending the widespread availability of the Summary Care Record it would be wise for those with a serious condition or adverse drug reactions to improvise one.
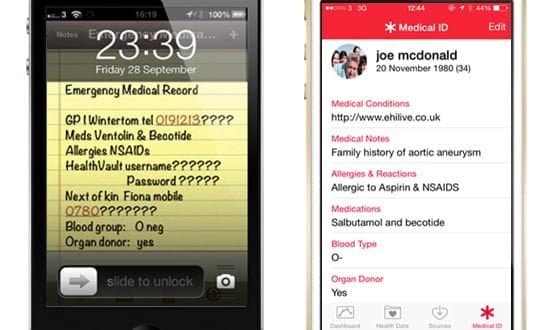
I suggested that people in this position should make an SCR visible on the front of their iPhone; writing it in the notes app and then screen-shotting it so that it could be set as the lock screen. It gladdened my heart that quite a few of you took the trouble to follow my advice.
When I downloaded iOS 8 to my iPhone, I was delighted to see that the new HealthKit app now includes the ability to click through the phone’s lock screen to an emergency medical record, ‘Medical ID’ (pictured).
This includes information on key diagnoses and allergies that could be accessed by anybody coming across an unconscious patient.
The information is obviously entered by the holder of the phone, and they enter it in the hope it might help them in an emergency. Therefore, they have, by virtue of the process, given consent for it to be viewed in an emergency.
Keeping the three privacy tribes happy
I have previously described three tribes in the SCR privacy concerns battle as the “couldn’t care less”, the “privacy zealots” and the “digital cavaliers”. In this context, I was struck by the power of Apple’s intrinsic consent model.
The “couldn’t care less” wouldn’t bother with the app and would enter no data – but, maybe, years down the line after a myocardial infarction, say, they might join the “digital cavaliers” and enter copious data.
The “privacy zealots” get to keep their data to themselves by not entering any data and indeed, deleting the app; again with the freedom to change camps should their health needs change. Simples.
But what if I have a really complicated medical history? Or I have a complex medication regime and I want my emergency carers to have access to my SCR?
Why not allow patients to insert a hyperlink into the app’s emergency information (Medical ID) screen that will display the SCR? This would put it, potentially, into the hands of anyone who needs it – at no cost to the NHS and with the patient deciding on consent.
In fact, why not let the “digital cavalier” with a complex condition and a good understanding of information governance have a link to their own, detailed care record?
The setting up of the app (Medical ID) and the choosing of what links to display on it effectively describe the user’s own assessment of the cost benefit analysis of sharing health data in an emergency.
A hyperlink will only get you so far
Anyway, I eagerly I entered a hyperlink instead of text into the medical conditions field of the app on my own phone and locked it.
Pressing the emergency button on the lock screen clicked me through to the Medical ID page, but tapping on the link did not take me through to a website.
Thinking about it, I guess it’s obvious that you may not want people to access your data connection through your lock screen; because you could end up with a big data bill if your phone was stolen and the internet accessed.
On the other hand, maybe that’s a risk worth taking for some. The point is that these decisions are highly individual and the appropriate level of consent to share fluctuates over time and by patient need. One size fits all, patently, doesn’t work.
Apple means slick
I recently attended an event in Leeds run by the Northern Health Science Alliance and Apple, where I learned more about Apple HealthKit.
It is a formidable undertaking by Apple, designed to take a great deal of health data from many sources, with the makers of, say, blood glucose monitors being encouraged to develop apps that will interface with it.
The day included a description of Apple’s work at the Mayo Clinic in the US (iPad usability out-front, with Cerner in the back-end, to paraphrase a considerably longer pitch).
It also included a description of Apple’s collaboration with Emis, which is using HealthKit to provide a personal health record to patients that GPs can view through Emis Web. This is very timely given the current commitments to give patients access to their own records.
One way and other, it did get me thinking: “Hmmmmm… maybe if you want gorgeously usable systems in health IT, the sensible thing to do is to get Apple to do the front end?” Who better?
But it doesn’t always play
Interested in learning more about HealthKit, I dropped heavy hints to Fiona in the run-up to Christmas about getting a fitness activity monitor.
I suggested that this would avoid my ever needing a paramedic to access my SCR, by encouraging me to be active and get all passionate about my weight and blood pressure.
Santa duly brought me a wrist worn pedometer called ‘Jawbone Up 24’. Unfortunately, my Jawbone wouldn’t talk to HealthKit because Apple appears to have done a deal with a rival piece of kit by Nike – or it may be waiting for the Apple Watch wearable.
Interoperability issues spiked my New Year fitness regime on day one. Foiled again. Maybe next year.
Time for Apple and the NHS to talk
Still, that smartphone lock screen continues to hold out the potential for every patient to set their healthcare records privacy sliders exactly where they want them in an emergency.
Perhaps while they’re at it, they could be asked where they’d like their privacy sliders set for care.data as well?
The growth of the SCR has been phenomenal over the last year. In fact, just this week it was announced that there are now 50 million SCRs in existence.
Accessing the SCR at the right place and time is now the key to its utility; so it’s time to put it in the patient’s pocket and hence the paramedic’s hand. Could Apple and the SCR team talk to each other? Preferably before my first myocardial infarction.
Given the rapid development of patient access to records online, with clear targets being set and enforced , the SCR will need a patient-centred smartphone access app to stay relevant.


Joe McDonald
Joe McDonald is a practising NHS consultant psychiatrist. Over the past five years he has been an NHS trust medical director and national clinical lead for IT at NHS Connecting for Health – a stint that included 18 months as medical director of the Lorenzo delivery team!
His experiences in the National Programme for IT in the NHS have left him with a passion for usability and "end user knowledge networks.” He is the founding chairman of the National Mental Health Informatics Network. Motto: we don't get fooled again. Follow him on twitter @CompareSoftware