Nervecentre’s EPMA goes live at Nottingham University Hospitals
- 23 June 2023
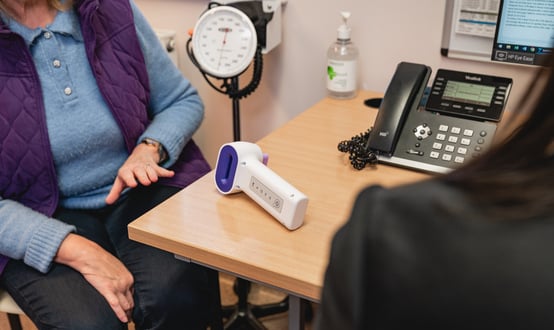
Nottingham University Hospitals (NUH) have deployed Nervecentre’s electronic prescribing and medicines administration (EPMA) solution to improve safety, advance its digital maturity, and provide real-time insight into prescribing activities.
The City Hospital (City) and Queen’s Medical Centre (QMC) were transitioned from paper drug charts to Nervecentre over two weekends, with City going first on May 20 and QMC following three weeks later on June 10.
The QMC go-live took place over the hottest weekend of the year and immediately before a three-day junior doctors’ strike. For QMC, the drug charts covering 14,100 prescriptions for more than 800 patients across 40 wards were transcribed into Nervecentre over two days.
Clinicians and operational teams at Nottingham University Hospitals NHS Trust were already heavy users of Nervecentre for a broad set of functionality, including viewing test results, vital signs, clinical noting, hospital at night, sepsis alerts, risk assessments, fluid balance, bed management and porterage.
Adding medication management and discharge summaries helps clinicians by consolidating all the information they need in one place – their mobile device.
Later this year, NUH will add ordering of investigations and the full suite of Emergency Department functionality to further consolidate its digital footprint.
Nervecentre’s EPMA allows users to prescribe and administer medicines using mobile devices, utilising closed loop barcode scanning of patient wristbands and medicines to ensure the safest practice at the patient’s bedside and leverage NUH’s investment in 12,000 mobile devices.
This mobile-first approach provides clinicians with live information about their patients and their medication and is proven to save time and improve safety and usability.
The new system helps to bolster prescribing confidence with automated decision support that includes the use of the BNF and Stockley’s drug-drug interactions, SNOMED and dm+d.
Clinical decision support draws upon allergies, height/weight, VTE assessments, vital signs and pathology results that are already present in Nervecentre.
It supports FHIR compliance, and information is shared with GPs using Nervecentre discharge summaries delivered over MESH, as well as shared with community pharmacies through integrated support for PharmOutcomes messaging.
Early feedback positive
Feedback has been positive from the start of the go-live. Doctors have said that EPMA makes their life easier and improves safety, and nurses appreciate the ability to have all information together in one place instead of wasting time looking for paper charts.
Mark Simmonds, deputy medical director at NUH, said: “The e-prescribing digital solution allows 24/7 access to a patient’s medication record from anywhere and will revolutionise the current paper-based medicine management processes.”
Paul Volkaerts, CEO at Nervecentre Software, added: “We are seeing evidence that a progressive deployment of an EPR delivers high levels of clinician buy-in from the outset, without the need for a stabilisation period.
“NUH has focused upon usability – ensuring their staff have tools that are easy to learn and to use, and allow them to spend more time caring for patients – and are reaping the rewards of that through strong levels of clinician adoption and satisfaction.”