Big EPR Survey reveals components of EPR
- 16 May 2013

EHI readers believe that the government should maintain a clear focus on electronic patient records as it pursues its vision of ‘paperless’ working.
Readers who completed The Big EPR Debate Survey rated PAS, clinical noting, order communications, pathology and eprescribing as the highest priority building blocks of an EPR.
Clinical decision support and advanced scheduling were given a low priority, as blocks that could wait.
Health secretary Jeremy Hunt has said that he wants the health service to be paperless by 2018, and has clarified this by saying that he wants to see it using electronic records and communications by this date.
Respondents to The Big EPR Survey, which EHI has just run as part of The Big EPR Debate, said that promised guidance, due in June, should provide much greater clarity on electronic patient records and what paperless actually means.
Nine out of ten (90.2%) of the 264 respondents said “we need to be clear about what we mean by phrases such as EPR” and that NHS England should define its terms.
Almost nine out of ten respondents (88.5%) also felt that “a paperless NHS requires EPRs “as a pre-requisite”.
The implication is that simply scanning documents, giving users ‘views’ of siloed information, and what one reader called “single-issue apps”, should not count as achieving the government’s goals.
EHI editor Jon Hoeksma said: “The Big EPR Survey clearly shows that EPRs remain the bedrock of digital healthcare in hospitals and beyond, and critical to patient safety and integrated care. While much attention is rightly focused on secondary uses of data there is still a big job to be done in ensuring the core clinical systems that will most directly impact frontline patient care are not ignored."
"NHS England needs to provide support and a road map on EPRs to help trusts ensure they have the building blocks of a safer more responsive digital NHS. Hospital EPRs are the foundations for a paperless NHS that still need to be completed."
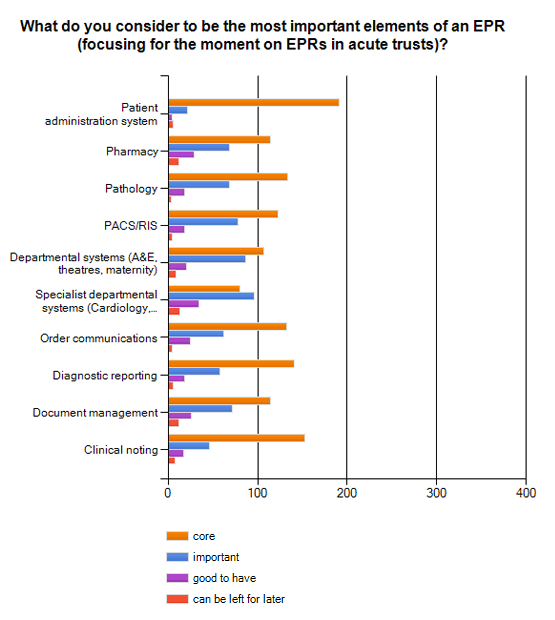
The Big EPR Survey asked readers to rate 15 systems that might be counted as part of an EPR in order of importance.
More than one in eight readers (85.3%) rated a patient administration system as a “core” element of an EPR.
After the PAS, almost seven out of ten readers (68.3%) suggested that clinical noting was a “core” part of an EPR while around six out of ten said that diagnostic reporting (62.9%), pathology (59.4%, order communications (58.9%), and e-prescribing (57.6%) should be counted as “core.”
Systems that readers felt could be “left for later” included systems to run hospitals more efficiently and, possibly, safely, such as patient level information costing systems (20.5%), clinical decision support systems (12.9%) and advanced scheduling (9.4%).
When asked about the route that hospitals should take in getting these different systems in place, there was a fairly even split between those who thought that trusts should use a single supplier for all elements or all core elements (17.1% and 31.1%) and those who thought they should adopt a pure ‘best of breed’ approach (42.8%).
A number of free text comments argued that the approach would depend on the trust’s digital development, but that it was essential for systems to work together. Despite the NPfIT experience, a number of readers also suggested that a single supplier approach was the safest way to achieve this.
“Integrated systems exploit clinical decision support, but some systems will need to be interfaced – eg PACS – in the short term,” one wrote.
“Over time, a trust would replace its legacy investment with one, integrated solution. There is no means for the foreseeable future of interfacing clinical decision support rules between systems,” another agreed.
EHI is running The Big EPR Debate to give readers a chance to shape the future of electronic records and a paperless NHS. What should NHS England’s guidance cover? What is an EPR? What is essential and what can be left for later? What should the next steps be. Join the debate.




