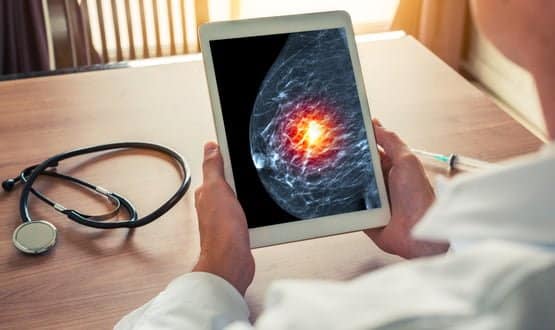
Two trusts have turned to artificial intelligence to help them spot patients with breast cancer earlier.
United Lincolnshire Hospitals NHS Trust (ULHT) and Nottingham University Hospitals Trust (NUHT) are taking part in a trial in conjunction with East Midlands Radiology Consortium (EMRAD) and UK-based AI companies Faculty and Kheiron Medical.
The trial aims to help develop, test and ultimately deploy artificial intelligence (AI) tools in the breast cancer screening programme in the East Midlands.
Kheiron Medical’s mammography intelligent assessment (MIA) uses AI algorithms to flag potential cases of breast cancer. It has been trialled in hospitals in Hungary, but the trial with ULHT and NUHT is the first UK trial.
The first phase is a retrospective trial using old images that have been anonymised to see how accurate MIA is at diagnosing scans that need further investigation.
The results will then be compared to the results produced by the breast screening reading team. Already, it is performing better than most humans, according to ULHT.
If it’s deemed safe, the next phase of the trial will see radiologists use MIA for the first read on all scans before they are reviewed by experts.
If there is any difference of opinion then the scan will automatically be sent for a third read.
Bernadette Trzcinski, ULHT consultant mammographer and the trust’s lead on the project, said: “Across the country we desperately need something to help us with the current staff shortages, which are predicted to become increasingly challenging as the demand for imaging grows.
“The success of this project will transform the breast screening service, improving both quality and efficiency for our breast screening population.
“It is not about replacing radiologists. All scans at the trust will continue to be read by at least one member of the breast screening reading team.
“However, if MIA is successful, it has the potential to half the amount of time we spend reviewing scans, this is time we could be spending with our patients, improving their overall experience.”
Dr Jonathan James, consultant radiologist at NUHT, added: “There is a shortfall in the number of trained radiologists nationally, with breast radiology particularly badly affected as in next five years for every two radiologists who currently join the screening programme, three are predicted to retire.
“The new MIA tool could replace one of those readers so that more of our radiologists are freed up to see women more quickly, reduce waiting times and help improve the overall patient experience.”
The trial will also use Faculty’s Platform software to optimise clinic scheduling and staff resourcing to make use of radiologists time.
The EMRAD programme, launched in 2013, saw the East Midlands become the first area where mammograms and diagnostic images could be shared quickly and easily between trusts in the region.
Currently, all images produced during breast screenings, known as mammograms, are reviewed by two members of the breast screening reading team.
But the national shortage of radiologists marks a clear need for alternative solutions to manage high levels of diagnostic scans in a timely manner.
Artificial intelligence has proven successful in helping clinicians spot a number of conditions.
Earlier this year, a team the University of Warwick developed an AI system that recognises radiological abnormalities in chest x-rays. The team said it could cut the time it takes to assess critical chest x-rays from 11 days to less than three.
The University of Surrey has also developed AI technology that can identify and help reduce the occurrence of urinary tract infections in dementia patients, helping keep them out of hospital by monitoring the condition remotely.
Earlier this month the Government announced £250 million for a National AI Lab to improve diagnostics and screening. The lab will be used to develop treatments for cancer, dementia and heart disease.
But the technology won’t solve all healthcare problems, some have warned. A report from the Academy of Medical Royal Colleges in January called for a line to be drawn to establish accountability between AI and clinicians.