Data Strategy: Patients to get easier access to medical data through NHS App
- 22 June 2021
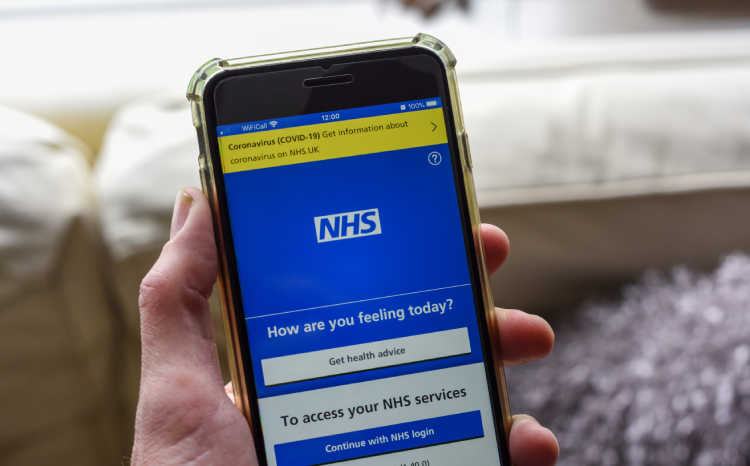
Patients are set to get easier access to their medication lists and care plans through the NHS App under the government’s new data strategy.
New requirements for data sharing across the entire health and care system are also set to come into place, with new legislation to be introduced to require all adult social care providers to provide information about the services they fund.
Published today (June 22), the NHSX draft strategy ‘Data Saves Lives: Reshaping health and social care with data’, aims to capitalise on the work undertaken using data during the pandemic to improve health and care services.
In a bid to establish openness, the government committed to publishing the first transparency statement setting out how health and care data has been used across the sector by 2022.
Under the proposals, patients are set to gain more control over their health data, while data will also be used to improve care and treatment.
Patients will be able to access their test results; medication lists; procedures; and care plans from across all parts of the health system through patient apps, such as the NHS App. This will be done by ensuring data is shared safely and more effectively across the system, according to a statement from the Department of Health and Social Care (DHSC).
It is also hoped that by improving access to data, people will be able to manage appointments, refill medications and speak with health and care staff when needed.
NHS organisations will be required to share anonymous data “safely and appropriately” to boost patient care and treatment under the strategy.
The strategy aims to break down data barriers and give patients confidence that health and care staff have up-to-date medical information, enabling clinicians to make quicker, more informed decisions to deliver better treatment, DHSC said.
Collating data into an easy to access system will help ensure NHS staff spend less time looking for the information they need, freeing them up to spend more time with their patients.
Health secretary, Matt Hancock, said: “More effective use of data will deliver better patient focused care. It will free up staff time to focus on patients and allow clinicians to make better, more informed decisions on treatment and support.
“This strategy seeks to put people in control of their own data, while supporting the NHS in creating a modernised system fit for the 21st century which puts patients and staff in pole position.”
The strategy will build on work such as the NHS Covid-19 Data Store, which was set up as a front door for access to data during the pandemic, with the aim to reduce red tape around data and information governance.
It promotes the use of technology including robotic process automation, which uses bots to automate back-office processes. It is expected to save the NHS more than half a million hours a year in staff time by 2025, according to a statement from DHSC.
It also includes proposals to make the UK a leader in innovation-friendly regulation of AI technologies. This will focus on developing unified standards for the efficacy and safety testing of AI solutions and streamlining the path to market AI technologies.
[themify_box icon=”info” color=”gray”]
The strategy aims to:
- put patients at the heart of their health and care data, with easy access to their own healthcare records
- give health and care staff easier access to the right information to provide the best possible care through shared records and simplified information governance
- enable the proportionate sharing of data for the purpose of supporting the health and care system
- give adult social care high quality, timely and transparent data so they can make individualised choices to personalise care
- modernise data architecture and infrastructure underpinning the health and care system to improve standards, protect data and stay ahead of cyber risk
- support innovation for the benefit of patients and staff, including the use of artificial intelligence
- build on improvements to speed up access to data during the pandemic, where there is clear benefit for the system as a whole
[/themify_box]
The draft strategy has been published ahead of a consultation with the public and stakeholders over the summer.
Matthew Gould, NHSX chief executive, said: “If we want to continue improving care, we need to transform how we use data. Patients need to own their data, have access to their data, and have confidence on how the NHS is handling it on their behalf.
“This strategy takes this agenda firmly forward, and is good news for patients, staff, citizens and anyone who cares about the future of the NHS.”
Dr Clare Gerarda, a GP and former chair of the Royal College of GPs, added: “Better use of data in health and care will be transformational to our NHS, to research, and is vital in our fight to reduce health inequalities and address unnecessary variations in care.
“Thanks to increased use of data and digital technologies, the NHS and general practice will come out of the pandemic better equipped to deliver more responsive services to patients, and this strategy will only help strengthen the care we can provide to the public.”
Transparency track record
The government’s use of data during the pandemic has faced criticism, particularly around transparency of contracts and scope for which data can be used by big tech firms.
A damning National Audit Office report on procurement during the pandemic found a general lack of transparency and adequate documentations around key decisions “such as why particular suppliers were chosen or how government identified and managed potential conflicts of interest”.
Contracts that have caused concern among tech justice advocates are those relating to AI firms Palantir and Faculty and their role in the NHS Covid-19 Data Store.
Most recently NHS Digital came under fire for its General Practice Data for Planning and Research (GPDPR) and the timeframe GPs had to implement it. GPDPR aims to give planners and researchers faster access to pseudonymised patient information.
NHS Digital announced in May 2021 that the new service would come into effect on 1 July 2021, with people given until 23 June to choose to opt out. After facing backlash from patients, doctors and health charities the deadline was moved to 1 September 2021.